Utah Insurance Department Updates: What Billing Partners Need to Know
August 5, 2025

Anyone working in the insurance billing industry needs to stay up to date on regulatory changes.
Recent updates from the Utah Insurance Department could have important implications for billing partners, affecting everything from compliance requirements to operational procedures.
Whether you work as a member of a revenue cycle management team, a healthcare administrator, or a third-party billing provider, being aware of these changes can help ensure seamless operations and reduce the risk of costly errors.
With regular updates from state organizations and payers—including Utah Medicaid, SelectHealth, and the Utah Insurance Department—Utah’s insurance market is constantly evolving.
For healthcare billing professionals, these changes directly impact how claims are processed, when reimbursements are made, and how credentialing affects network status.
In this blog, we will break down the latest updates and explain what they mean for your practice.
For medical billing professionals in Utah, understanding state insurance regulations is essential—not optional. The Utah Insurance Department directly influences claim submission processes, denial management, and credentialing maintenance. With evolving rules around prior authorizations, electronic submissions, and provider data accuracy, even minor compliance gaps can result in delayed payments or audit risks. Staying informed about regulatory changes not only protects revenue but also ensures billing workflows align with payer expectations and legal requirements across both Medicaid and private insurance plans.
Billing professionals must understand Utah’s insurance laws to avoid claim denials and ensure timely reimbursements.
The Utah Insurance Department enforces specific regulations, including a requirement that insurers make claim decisions within 30 days of submission.
Missing certain deadlines—whether due to billing errors or payer delays—can result in automatic denials or delayed payments, directly affecting provider revenue cycles. Additionally, Utah’s insurance laws often contain provisions that differ from federal requirements.
To maintain compliance and avoid costly administrative burdens from appeals or resubmissions, billing teams must be aware of these state-specific variations.
Utah Medicaid and SelectHealth, like other insurance payers, regularly update their credentialing criteria, modifier validations, and claim processing systems.
If billing partners are not properly informed or prepared for these changes, it can lead to claim delays or denials. For example, recent updates to the Utah Health Information Network (UHIN)—which facilitates electronic claims—have temporarily disrupted operations, resulting in duplicate claim submissions and missing acknowledgements.
These types of technical issues often cause increased denial rates until they are resolved.
To address systemic issues and minimize revenue loss, billing staff should monitor official system status notifications, regularly review denial trends, and establish proactive communication strategies with payers.
Federal guidelines—such as those set by CMS—form the foundation for claims processing and credentialing. However, Utah Medicaid enforces additional state-specific requirements.
For instance, Utah Medicaid mandates that providers enroll through UHIN’s trade partner system before submitting claims, even though this is not a federally mandated step. The state also has unique audit requirements regarding the use of modifiers and diagnosis codes, which may not align fully with CMS regulations.
To ensure that claim submissions meet all local compliance standards, billing teams must stay informed about these state-specific rules and regularly consult Utah Medicaid’s provider manuals and payer instructions. Failure to comply with both federal and Utah-specific requirements can lead to denials or payment delays—ultimately affecting cash flow and provider satisfaction.
In 2024, Utah implemented H.B.495, which reinforced existing state rules around claim processing timelines. Billing partners must stay aware of law updates, policy updates, and procedural changes affecting both public and private payers in order to maintain compliance with Utah’s changing insurance sector. Several legislative changes were implemented in 2024 that have an immediate impact on payer procedures, provider communications, and claim reimbursement.

In 2024, Utah introduced several new mandates and policies aimed at enhancing accountability and efficiency in healthcare reimbursements. These regulations impact how providers submit claims, fulfill credentialing requirements, and respond to denials. With stricter appeal timelines and an increased focus on electronic submissions, the changes are designed to reduce fraud, improve accuracy, and ensure timely payments. For billing professionals, understanding and adapting to these mandates is essential to maintaining compliance and optimizing revenue cycles.
H.B. 495 – Claim Processing Timelines:
This law upholds state regulations that mandate insurers respond to clean claims within 30 days of receiving them, either by paying them or rejecting them. A 15-day extension might be allowed if more time is required, but only after providers are notified in advance. It might require up to 45 days for insurers to make a final decision in situations where provider information is not accessible. The purpose of this bill is to improve payment procedures’ reliability and transparency while addressing frequent payment delays.
SB 196 – Physical Therapists as Primary Care Providers:
Nowadays, physical therapists have the same status as primary care physicians. When PTs are chosen as the primary care option, insurers are not allowed to impose differential billing or increased patient cost-sharing.
HB 301 – Ambulance Service Payments:
Balance billing for out-of-network ground ambulance transportation is eliminated since insurers are required to pay ambulance providers directly. Without charging patients for outstanding finances, providers must work with insurance to arrange payments.
Effective communication between healthcare providers and payers is crucial for smooth billing operations. In 2024, Utah’s major insurers have enhanced their communication protocols to improve transparency and streamline issue resolution. These updates include more timely notifications about claim denials, clearer guidelines for submitting additional documentation, and expanded use of electronic portals and automated messaging systems. Staying up to date with these changes helps billing partners respond more quickly to payer requests and reduces the risk of delayed payments.
As of Q1 2024, the Utah Insurance Department mandated that payers
In 2024, several key updates from Utah’s major payers—including Utah Medicaid, Anthem, SelectHealth, and Molina—are reshaping how healthcare providers manage billing and claims. These changes include new claim submission formats, stricter credentialing processes, revised denial management protocols, and updated timelines for approvals and appeals. Staying informed about these payer-specific updates is critical for billing partners to maintain compliance, reduce denials, and ensure timely reimbursement in Utah’s evolving healthcare landscape.
Utah Medicaid
SelectHealth
Anthem & Molina
As healthcare regulations evolve in Utah, billing teams must adapt to new requirements introduced by the Utah Insurance Department, Utah Medicaid, Anthem, and Molina. These changes are impacting the revenue cycle in several ways, including claim filing procedures and document management. Understanding these updates is essential to minimize denials, ensure compliance, and maintain timely reimbursement. The main areas affected by the 2024 policy and system upgrades are outlined below:
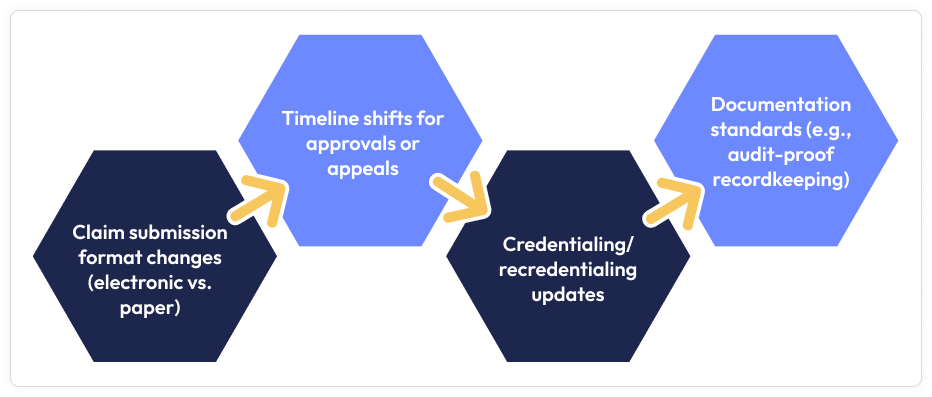
Utah Medicaid and private payers, including SelectHealth and Molina, now require electronic claim submission in the X12 837 format. Although paper claims are still occasionally accepted, they are more likely to be denied or delayed. Electronic submission enables better tracking, faster processing, and fewer errors. To remain compliant and avoid reimbursement challenges, billing teams that have not yet fully transitioned to electronic data interchange (EDI) should make the switch immediately.
New regulations, such as Utah’s SB 274, require payers to notify providers at least 30 days in advance of any changes to prescription formulas or pre-authorization procedures. While billing teams must stay vigilant for payer updates, this notice period also gives providers more time to adjust. Additionally, payers like SelectHealth have expedited appeals processes, reviewing urgent cases in as little as 72 hours. The standard 60-day appeal window remains in effect. These changes highlight the need for internal systems that track deadlines and respond promptly to prior authorization requirements or claim denials.
Utah Medicaid now uses the PRISM portal for all provider enrollment and updates, with credentialing procedures moving to digital platforms. All providers must maintain current and accurate information on this new platform to avoid claim denials and continue providing services. Meanwhile, private payers like SelectHealth and Anthem regularly update provider lists and rely on CAQH or their own portals to verify credentials. To ensure billing privileges are maintained and practices operate smoothly, organizations should designate someone to periodically review NPI numbers, licenses, and group affiliations.
With automated audits highlighting incorrect or missing data, payers throughout Utah are placing greater emphasis on documentation quality. For example, denials often result from ICD-10 code mismatches, such as “excludes 1” errors. Billing teams are now responsible for ensuring that all claims include accurate diagnosis and procedure codes, authorization details, and supporting documentation. Effective documentation not only safeguards procedures during payer audits but also ensures compliance. It is recommended that all billing documents, including detailed records of all insurer correspondence, be securely stored for at least six years.
As Utah’s healthcare billing environment becomes increasingly complex, billing teams must understand the unique policies and procedures of major payers such as Utah Medicaid, SelectHealth, and Molina. These payers have introduced new systems, updated compliance standards, and implemented stricter deadlines for claims and appeals. While these changes raise the stakes for accuracy and timeliness, they are designed to improve efficiency and oversight. Maintaining smooth reimbursement workflows and preventing avoidable denials depends largely on staying aligned with each payer’s expectations.
In 2024, Utah’s three major healthcare payers—Utah Medicaid, SelectHealth, and Molina—each adopted significant compliance changes that immediately impacted billing operations. Utah Medicaid fully implemented the PRISM system, a unified platform for provider enrollment, claims, and prior authorizations. To continue receiving reimbursement, all Medicaid providers must maintain up-to-date information in PRISM. Among private payers, SelectHealth leads the industry with strict electronic claims guidelines that require the use of UHINs for submissions and remittance tracking. Its credentialing process is closely tied to CAQH profiles, which are regularly reviewed and verified. Molina complies with state-mandated laws under SB 274, which requires all insurers to provide providers with 30 days’ notice before changing prior authorization or formulary regulations, although its changes receive less widespread attention. As these changes take effect in May 2025, billing teams must remain vigilant to payer updates.
In 2024, common reasons for claim refusals among Utah’s three main payers include missing or expired prior authorizations, inaccurate or outdated credentialing information, and mismatched procedure-to-diagnosis coding. Since the launch of PRISM, Utah Medicaid has occasionally experienced backlogs, particularly among providers still adapting to the new submission processes. Automated denial systems quickly flag incomplete claims, often before human review. While most standard denials receive a decision within 15 to 30 days, SelectHealth has shortened response times for urgent appeals, resolving cases in as little as 72 hours. Molina typically takes longer, especially when handling out-of-network providers or secondary claims. Delays in follow-up or missing documents can result in denials that are difficult to overturn, making it crucial to file appeals promptly.
By ensuring they have the latest tools and workflows tailored to each insurer’s platform, billing partners can stay aligned with Utah’s payer systems. All Medicaid enrollments, updates, and claims processing must now be completed through the PRISM portal. Errors in license information or NPI data can lead to denials that won’t be reimbursed until corrected. Maintaining an active UHIN link is essential for SelectHealth and Molina, as this system handles electronic claim submissions, eligibility verifications, and remittance distribution. Additionally, because payers like SelectHealth rely on CAQH to verify ongoing provider eligibility, credentialing should be reviewed regularly. Keeping these systems up to date enables billing teams to respond promptly to updates, system issues, or changing prior authorization requirements, while also preventing denials.
Billing partners must be proactive to keep pace with the Utah Insurance Department’s ongoing regulatory changes and the evolution of payer systems like PRISM and UHIN. In today’s billing environment, compliance goes beyond submitting accurate claims; it requires staying informed, adaptable, and skilled in technology. Whether working with Molina, Utah Medicaid, or SelectHealth, anticipating payer expectations can accelerate reimbursements, minimize credentialing disruptions, and significantly reduce denials. The following strategies outline how billing teams can remain effective and compliant amid Utah’s evolving healthcare landscape.
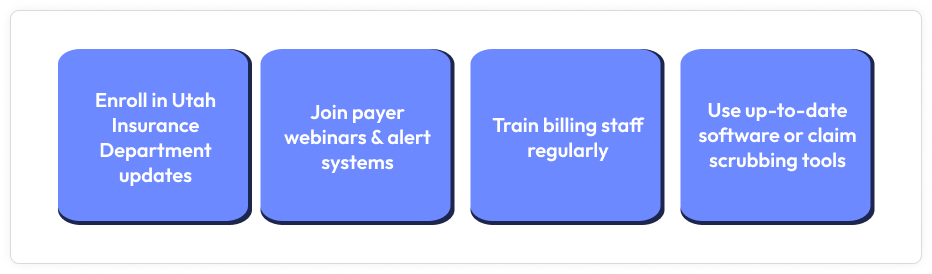
One of the best ways for billing partners to maintain compliance is by regularly collecting updates from the Utah Insurance Department. These updates include notifications about new laws (such as SB 274), changes to rules, audit standards, and insurance requirements that impact medical billing. By receiving information directly from the source, billing managers can stay ahead of changes before they take effect. This is especially important in a regulatory environment where strict compliance deadlines apply and missing critical information can lead to claim denials or penalties
To keep providers and billing teams informed, several Utah payers—including Molina, Utah Medicaid, and SelectHealth—offer webinars, newsletters, and real-time alert systems. These resources often cover credentialing updates, claim submission procedures, denial trends, and live demonstrations of new technologies. Attending such sessions gives billing partners the opportunity to ask questions and clarify any unclear policies, helping them stay aligned with each payer’s requirements. One simple way to reduce costly misunderstandings is to subscribe to email notifications and regularly check each payer’s provider portal.
Maintaining billing compliance and accuracy requires ongoing staff training. Utah’s billing and coding regulations are frequently updated, especially with changes to payer-specific requirements, PRISM, and claim formats like the 837. Regular internal training ensures that staff can identify issues that may lead to denials, such as coding errors, expired authorizations, or submission mistakes. Training should also include refreshers on appeal deadlines, new payer communication protocols, and documentation best practices to prepare teams for audits.
The use of integrated claim scrubbing tools and updated billing software is now mandatory. Outdated systems often fail to accommodate payer-specific regulations and new file formats, resulting in costly claim rejections. By leveraging claim scrubbing software, billing teams can save time by detecting errors—such as invalid NPIs, missing modifiers, and incorrect coding—before submission. Platforms that integrate with payer EDI or UHIN systems can significantly reduce delays and improve clean claim rates. Regular software updates also ensure that your staff can respond to payer changes in real time without interrupting workflow.
Utah billing services offer vital support to healthcare providers by leveraging deep local knowledge of payer regulations and compliance requirements specific to Utah Medicaid, SelectHealth, and other regional insurers. They use advanced claim scrubbing systems to identify and prevent denials before submission, increasing claim acceptance rates and streamlining reimbursements.
However, billing partners provide ongoing training to ensure staff stay informed about evolving audit requirements, credentialing processes, and payer regulations. As Utah’s healthcare billing landscape continues to evolve, this combination of expertise, technology, and education helps providers maintain financial stability and compliance.
Staying up to date with the latest Utah Insurance Department rules, regulations, and payer requirements is essential for smooth medical billing and timely reimbursements. To avoid costly denials and compliance issues, billing partners must remain proactive, knowledgeable, and technologically adept as private payers like SelectHealth and Utah Medicaid’s PRISM system continue to evolve. Providers can access the expertise and resources needed to navigate these complexities by consulting or partnering with experienced local billing services. By working with experts familiar with Utah’s unique healthcare landscape, providers can focus on delivering high-quality care while maximizing revenue.
FAQ’s
What is the role of the Utah Insurance Department in billing?
The Utah Insurance Department oversees and enforces state insurance laws and regulations, including those related to healthcare billing. It ensures that payers and providers adhere to billing standards, protects patient rights, and updates rules—such as credentialing requirements and claim submission protocols—to promote transparency and fairness in the reimbursement process.
How do I stay updated with changes?
To stay current with changes, providers and billing partners should subscribe to official Utah Insurance Department communications, participate in payer webinars offered by Utah Medicaid, SelectHealth, and Molina, and regularly monitor provider portals. Utilizing these resources enables billing teams to proactively adjust workflows and avoid disruptions caused by new regulations or system updates.
What are the most common billing mistakes in Utah?
Common billing errors include submitting claims with outdated credentialing information, missing or incorrect prior authorizations, and mistakes in claim formats or coding. These errors often lead to denials or delayed payments but can be minimized through regular training, the use of claim scrubbing tools, and staying up to date with payer-specific requirements.
Are electronic claims required now?
Yes, electronic claim submission has become the standard, particularly for Utah Medicaid and major private payers like SelectHealth. Platforms such as PRISM and UHIN facilitate these electronic transactions, and billing partners are encouraged to use them to ensure faster processing, minimize errors, and comply with state mandates restricting paper claim submissions